您好!欢迎访问洛阳富道生物科技有限公司官方网站!
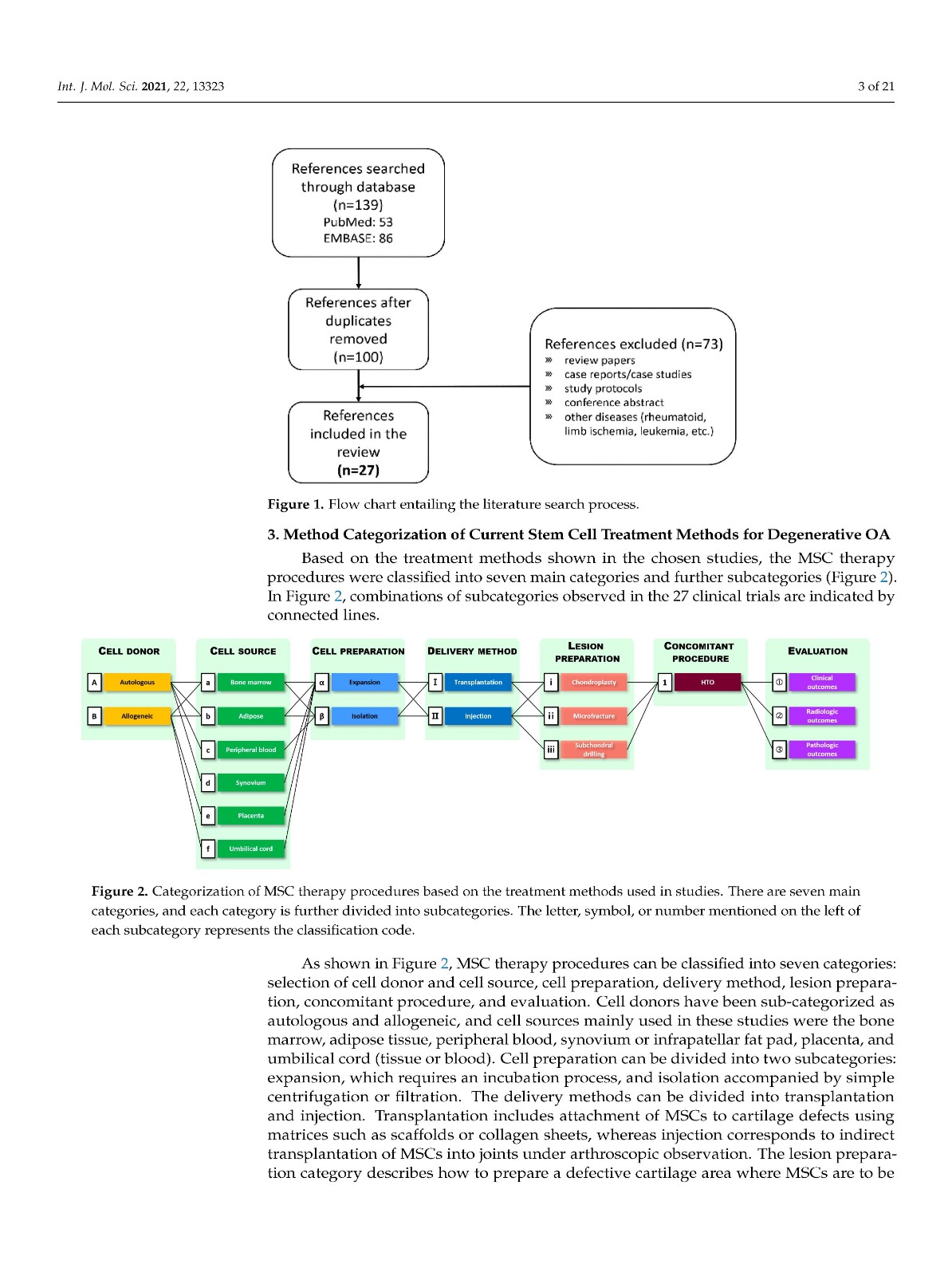
Current clinical applications of mesenchymal stem cell therapy for osteoarthritis lack consistency because there are no established criteria for clinical processes. We aimed to systematically organize stem cell treatment methods by reviewing the literature. The treatment methods used in 27 clinical trials were examined and reviewed. The clinical processes were separated into seven categories: cell donor, cell source, cell preparation, delivery methods, lesion preparation, concomitant procedures, and evaluation. Stem cell donors were sub-classified as autologous and allogeneic, and stem cell sources included bone marrow, adipose tissue, peripheral blood, synovium, placenta, and umbilical cord. Mesenchymal stem cells can be prepared by the expansion or isolation process and attached directly to cartilage defects using matrices or injected into joints under arthroscopic observation. The lesion preparation category can be divided into three subcategories: chondroplasty, microfracture, and subchondral drilling. The concomitant procedure category describes adjuvant surgery, such as high tibial osteotomy. Classification codes were assigned for each subcategory to provide a useful and convenient method for organizing documents associated with stem cell treatment. This classification system will help researchers choose more unified treatment methods, which will facilitate the efficient comparison and verification of future clinical outcomes of stem cell therapy for osteoarthritis.

The purpose of this study was to increase the consistency of future MSC therapies for OA by categorizing the current treatment methods.
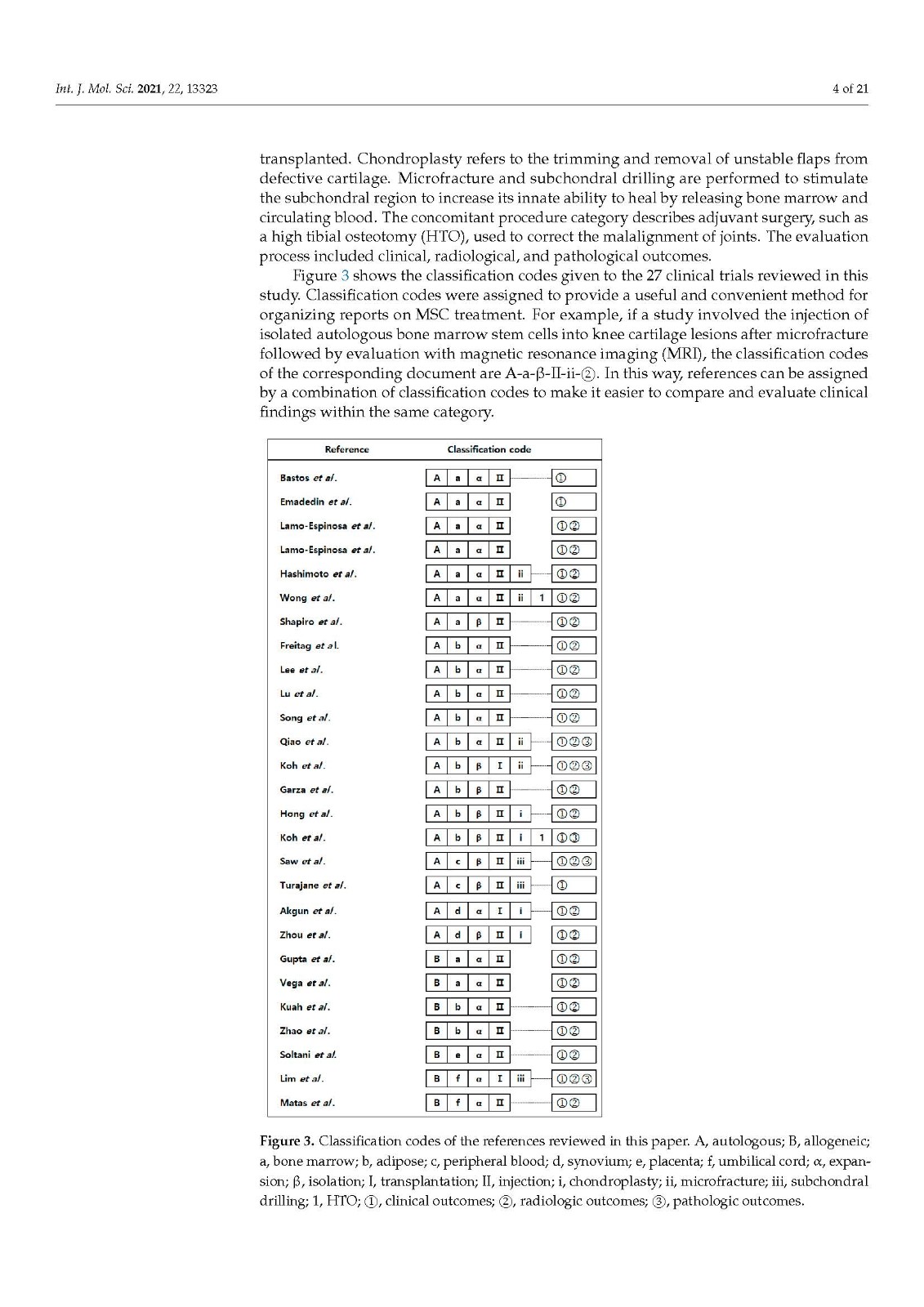
The treatment methods can be divided into seven categories: cell donor, cell source, cell preparation, delivery methods, lesion preparation, concomitant procedures, and evaluation. Based on these procedures, classification codes were assigned to each subcategory. Stem cell donors were subdivided into autologous and allogeneic, and stem cell sources included bone marrow, adipose tissue, peripheral blood, synovium, placenta, and umbilical cord. MSCs were prepared through cell expansion or isolation processes. They were attached to cartilage defects using matrices or injected into the joints under arthroscopic observation. The lesion preparation category was divided into three subcategories: chondroplasty, microfracture, and subchondral drilling. The concomitant procedure category describes adjuvant surgery, such as high tibial osteotomy.
Additional parameters can be added in future clinical studies. Cell sources can include MSCs from molar cells, amniotic fluid, and induced pluripotent stem cells. Some alternative cell sources, such articular cartilage progenitors and chondrogenic progenitor cells that have the potential to treat OA can also be considered as new parameters [74,75]. The addition of various treatment factors, such as PRP, hyaluronic acid, and some growth factors, can be considered as a new category. Low-intensity pulsed ultrasound (LIPUS), meniscectomy, and anterior cruciate ligament (ACL) reconstruction can be attempted as additional concomitant procedures. Since current MSC therapies are inconsistent and lack homogeneity, the classification system proposed in this study is expected to facilitate the efficient comparison and verification of clinical outcomes from MSC therapy for degenerative OA. Furthermore, if the analysis of the clinical results for each category is accumulated, the optimal combinations of efficient stem cell treatment methods can be found.

T75细胞培养瓶
本研究的目的是通过对当前治疗方法进行分类,提高未来 MSC 治疗 OA 的一致性。
治疗方法可分为七类:细胞供体、细胞来源、细胞制备、递送方法、病变制备、伴随程序和评估。根据这些程序,为每个子类别分配了分类代码。干细胞捐献者分为自体和异体,干细胞来源包括骨髓、脂肪组织、外周血、滑膜、胎盘和脐带。MSCs 是通过细胞扩增或分离过程制备的。它们使用基质附着在软骨缺损处或在关节镜观察下注射到关节中。病变准备类别分为三个子类别:软骨成形术、微骨折和软骨下钻孔。伴随手术类别描述了辅助手术,例如胫骨高位截骨术。
可以在未来的临床研究中添加其他参数。细胞来源可以包括来自磨牙细胞、羊水和诱导多能干细胞的 MSC。一些替代细胞来源,例如具有治疗 OA 潜力的关节软骨祖细胞和软骨祖细胞,也可被视为新参数 [ 74 , 75]]。各种治疗因子的加入,如PRP、透明质酸,以及一些生长因子,可以算是一个新的品类。可以尝试低强度脉冲超声 (LIPUS)、半月板切除术和前交叉韧带 (ACL) 重建作为额外的伴随手术。由于目前的 MSC 疗法不一致且缺乏同质性,因此本研究中提出的分类系统有望促进 MSC 治疗退行性 OA 的临床结果的有效比较和验证。此外,如果累积对每个类别的临床结果的分析,可以找到有效干细胞治疗方法的最佳组合。
关键词: 退行性骨关节炎,干细胞疗法,膝盖,软骨再生,degenerative osteoarthritis,stem cell therapy, knee, cartilage regeneration
来 源: MDPI https://www.mdpi.com/1422-0067/22/24/13323/htm
















上一篇: 细胞工厂内支原体污染的四种检测方法
下一篇: 血清瓶有哪些特点