您好!欢迎访问洛阳富道生物科技有限公司官方网站!
Clinical Studies on Cytokine-Induced Killer Cells: Lessons from Lymphoma Trials
细胞因子诱导的杀伤细胞的临床研究:淋巴瘤试验的教训
Lymphoma is a heterogeneous group of neoplasms including over 70 different subtypes. Its biological characteristic of deriving from lymphoid tissues makes it ideal for immunotherapy. In this paper, we provide insights into lymphoma-specific clinical trials based on cytokine-induced killer (CIK) cell therapy. We also reviewed pre-clinical lymphoma models where CIK cells have been used along with other synergetic tumor-targeting immune modules to improve their therapeutic potential. From a broader perspective, we will highlight that CIK cell therapy has potential, and in this rapidly evolving landscape of cancer therapies its optimization (as a personalized therapeutic approach) will be beneficial in lymphomas.
淋巴瘤是一组异质性肿瘤,包括 70 多种不同的亚型。其源自淋巴组织的生物学特性使其成为免疫疗法的理想选择。在本文中,我们提供了对基于细胞因子诱导的杀伤 (CIK) 细胞疗法的淋巴瘤特异性临床试验的见解。我们还审查了临床前淋巴瘤模型,其中 CIK 细胞已与其他协同肿瘤靶向免疫模块一起使用,以提高其治疗潜力。从更广泛的角度来看,我们将强调 CIK 细胞疗法具有潜力,在这个快速发展的癌症疗法领域,其优化(作为个性化治疗方法)将有益于淋巴瘤。

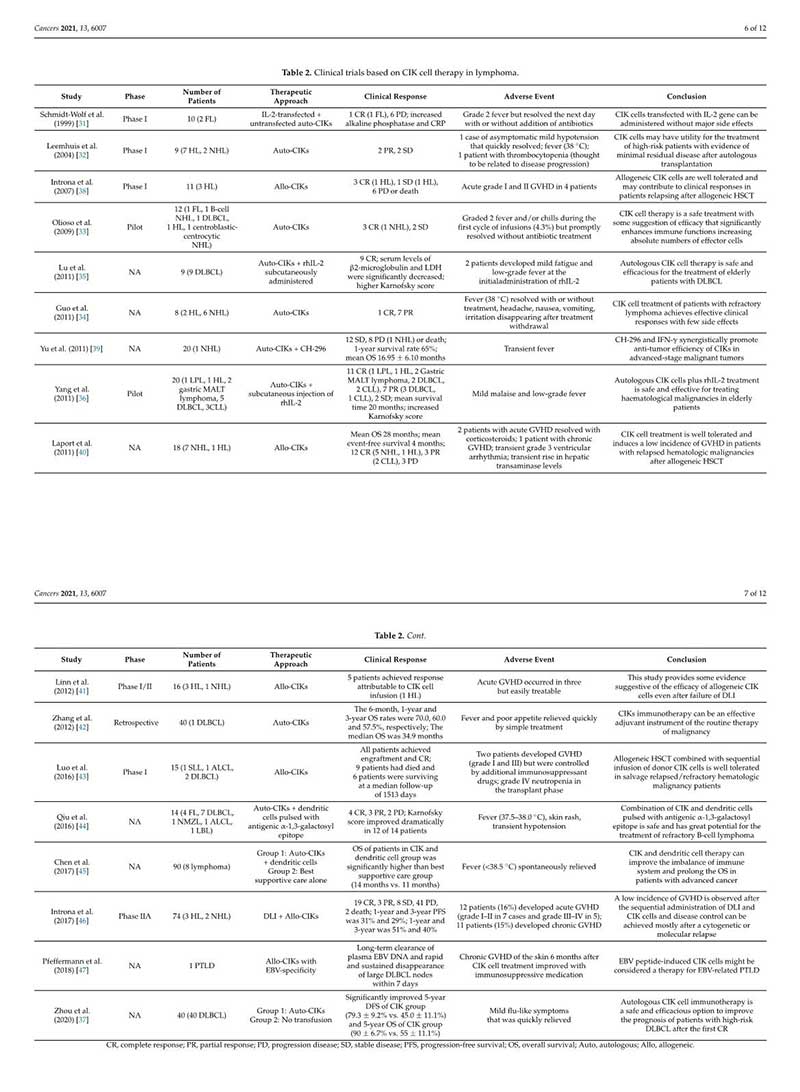
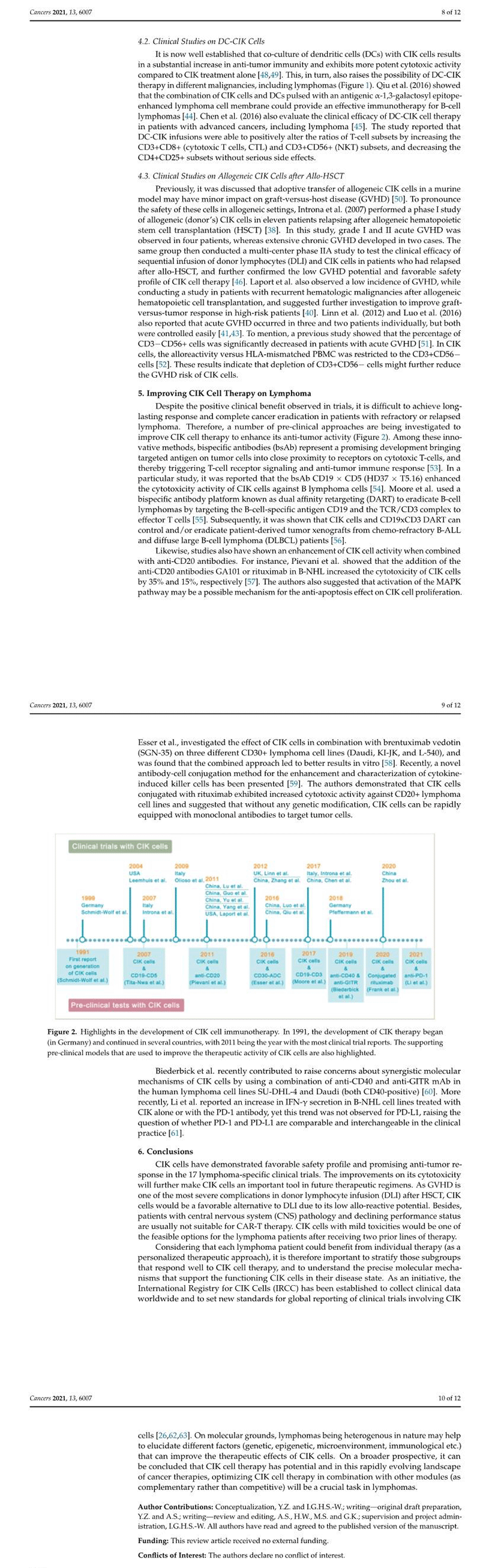
CIK cells have demonstrated favorable safety profile and promising anti-tumor response in the 17 lymphoma-specific clinical trials. The improvements on its cytotoxicity will further make CIK cells an important tool in future therapeutic regimens. As GVHD is one of the most severe complications in donor lymphocyte infusion (DLI) after HSCT, CIK cells would be a favorable alternative to DLI due to its low allo-reactive potential. Besides, patients with central nervous system (CNS) pathology and declining performance status are usually not suitable for CAR-T therapy. CIK cells with mild toxicities would be one of the feasible options for the lymphoma patients after receiving two prior lines of therapy.
Considering that each lymphoma patient could benefit from individual therapy (as a personalized therapeutic approach), it is therefore important to stratify those subgroups that respond well to CIK cell therapy, and to understand the precise molecular mechanisms that support the functioning CIK cells in their disease state. As an initiative, the International Registry for CIK Cells (IRCC) has been established to collect clinical data worldwide and to set new standards for global reporting of clinical trials involving CIK cells [26,62,63]. On molecular grounds, lymphomas being heterogenous in nature may help to elucidate different factors (genetic, epigenetic, microenvironment, immunological etc.) that can improve the therapeutic effects of CIK cells. On a broader prospective, it can be concluded that CIK cell therapy has potential and in this rapidly evolving landscape of cancer therapies, optimizing CIK cell therapy in combination with other modules (as complementary rather than competitive) will be a crucial task in lymphomas.

CIK 细胞在 17 项淋巴瘤特异性临床试验中显示出良好的安全性和有希望的抗肿瘤反应。其细胞毒性的改进将进一步使 CIK 细胞成为未来治疗方案中的重要工具。由于 GVHD 是 HSCT 后供体淋巴细胞输注 (DLI) 中最严重的并发症之一,CIK 细胞由于其低同种异体反应潜力将成为 DLI 的有利替代品。此外,中枢神经系统(CNS)病变和体能状态下降的患者通常不适合CAR-T治疗。具有轻度毒性的 CIK 细胞将是接受两种先前治疗后的淋巴瘤患者的可行选择之一。
考虑到每个淋巴瘤患者都可以从个体治疗中受益(作为一种个性化的治疗方法),因此对那些对 CIK 细胞治疗反应良好的亚组进行分层,并了解支持其疾病中发挥功能的 CIK 细胞的精确分子机制是很重要的状态。作为一项倡议,CIK 细胞国际注册中心 (IRCC) 已成立,旨在收集全球临床数据并为涉及 CIK 细胞的临床试验的全球报告制定新标准 [ 26 , 62 , 63]。在分子基础上,淋巴瘤本质上是异质的,可能有助于阐明可以提高 CIK 细胞治疗效果的不同因素(遗传、表观遗传、微环境、免疫学等)。从更广泛的角度来看,可以得出结论,CIK 细胞疗法具有潜力,在这种快速发展的癌症疗法领域,优化 CIK 细胞疗法与其他模块(作为补充而不是竞争)相结合将是淋巴瘤的一项关键任务。
关键词:lymphoma; cytokine-induced killer cells; clinical study; immunotherapy 淋巴瘤;细胞因子诱导的杀伤细胞;临床研究;免疫疗法
来源:MDPI https://www.mdpi.com/2072-6694/13/23/6007/htm

上一篇: 如何将胎牛血清分装到PETG血清瓶
下一篇: 细胞摇瓶培养灵芝对培养基的几点要求